Whereas age is a main risk factor for knee -osteoarthritis, young people can get it, too. For some people, it may be due to hereditary factors. For many individuals, it can happen due to injury or infection or even because of being overweight.
Read on here for answers to your questions about osteoarthritis of knee, including what is osteoarthritis, who are likely to get it, its causes, symptoms and treatments.
What Is Osteoarthritis?
Sometimes called as degenerative joint disease or degenerative arthritis, osteoarthritis (OA) commonly is known as wear-and-tear arthritis. It is a condition in which the natural cushioning, a firm, rubbery material between joints called as cartilage wears away. OA can affect any joint, but it occurs most often in knees, hips, lower back and neck, small joints of the fingers and the bases of the thumb and big toe.
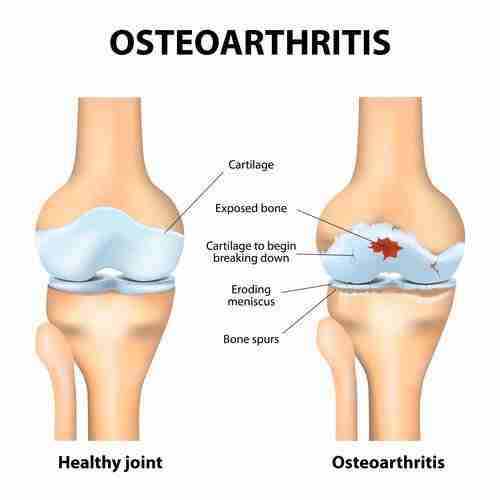
In OA, the cartilage breaks down and so the shock-absorbing capability of the cartilage gets impaired. Consequently, the bones of the joints rub more closely against one another with less of the shock-absorbing benefits of cartilage. This condition leads to pain, swelling , problems moving the joint and, sometimes, the formation of bone spurs. In the final stages of OA, the cartilage wears away and bone rubs against bone leading to joint damage and more pain.
Who Gets Osteoarthritis of the Knee?
Osteoarthritis is the most common form of arthritis. While it can occur even in young people, the chance of developing osteoarthritis rises after age 45. The disease affects both men and women. Before age 45, osteoarthritis is more common in men than in women. After age 45, osteoarthritis is more common in women. According to the Arthritis Foundation, more than 27 million people in the U.S. have osteoarthritis, with the knee being one of the most commonly affected areas.
What Causes Osteoarthritis Of The Knee?
The foremost cause of knee osteoarthritis is age. Almost everyone will eventually develop some degree of osteoarthritis. However, many factors can increase your osteoarthritis of the knee risk at an early age.
(i) Age: You’re in your late 40s or older. As you grow old your muscles gets weaker, your cartilage is less able to heal itself or your joints have gradually worn out over time.
(ii) Weight: You’re overweigh. This increases the chances of developing osteoarthritis and of it becoming gradually worse. Weight increases pressure on all the joints, especially the knees. Every pound of weight you gain adds 3 to 4 pounds of extra weight on your knees.
(iii) Heredity: If your parents or siblings have had osteoarthritis, you are more likely to develop osteoarthritis of the knee. It can also occur, if you were born with some abnormalities in the shape of the bones that surround the knee joint.
(iv) Gender: If you are a woman. Knee osteoarthritis is more common and more severe in women.
(v) Repetitive Stress Injuries: You do a hard, repetitive activity, a physically demanding job or a lot of physical activity, which can stress knee joint. Examples are squatting, or lifting heavy weights (55 pounds or more). They increase chances of developing osteoarthritis of the knee due to constant pressure on the joint.
(vi) Other Illnesses: You have another type of joint disease, which has damaged your joints. Examples are rheumatoid arthritis (the second most common type of arthritis) or gout. People with certain metabolic disorders, such as iron overload or excess growth hormone are at higher risk for developing osteoarthritis.
(vii) Athletics: Athletes involved in long-distance running soccer, tennis, are more likely to get osteoarthritis of the knee. That means athletes should take extra precautions to avoid injury.
Note: However, it’s important to note that regular moderate exercise strengthens joints and can decrease the risk of osteoarthritis. In fact, weak muscles around the knee can result into osteoarthritis.
What Are the Symptoms of Knee Osteoarthritis?
The main symptoms of osteoarthritis of the knee are:
(i) Pain: Particularly increases when you are active, moving your knee or at the end of the day. This usually gets better with rest
(ii) Swelling: Hard swellings (caused by osteophytes) or soft swellings (caused by extra fluid in the joint).
(iii) Stiffness: Stiffness in the knee, especially in the morning or when you have been sitting for a while. This usually eases after a minute or so as you get moving.
(iv) Creaking: Crackly sound that is heard when the knee moves or a creaking, crunching, grinding sensation when you move the joint.
(v) Decrease In Mobility Of The Knee: Your knee not moving as freely or as far as normal, making it difficult to get in and out of chairs or cars, use the stairs, or walk
(vi) Feeling of warmth in the joint
(vii) Your pain may vary and that you have good days and bad days, sometimes depending on how active you’ve been but sometimes for no clear reason.
(viii) Some individuals find that changes in the weather (particularly damp weather and low pressure) make their pain and stiffness worse. This could be due to nerve fibers in the capsule of their knee are sensitive to changes in atmospheric pressure.
How Is Osteoarthritis of the Knee Diagnosed?
Your doctor will first begin with a physical examination, take your medical history and note any symptoms. You also need to tell him what makes the pain worse or better to help your doctor ascertain whether osteoarthritis, or something else is causing your pain. If anyone else in your family has arthritis is also a relevant factor.
Your doctor will check for:
(i) tenderness over your knee
(ii) creaking and grating (crepitus)
(iii) bony swelling
(iv) excess fluid
(v) restricted movement
(vi) instability of your knee
(vii) thinning of the muscles that support your knee.
Your doctor may order additional tests for osteoarthritis of the knee, including:
(i) X-rays are the most useful tests to confirm a diagnosis of osteoarthritis, although they won’t often be needed. They can show narrowing of the space between bones, calcium deposits within your joint, bone and cartilage damage as well as the presence of bone spur. X-rays aren’t a good indicator of how much pain or disability you’re likely to have – some people have a lot of pain from minor joint damage but others have little pain from severe damage.
(ii) MRI scans may be required when X-rays do not give a clear reason for joint pain or when the X-rays suggest that other types of joint tissue could be damaged. MRI scan on your knee will show the soft tissues (e.g. cartilage, tendons, muscles) and changes in the bone that can’t be seen on a standard x-ray. This is quite rare though.
Note: There’s no blood test for osteoarthritis but they can be used to rule out other conditions, which might be causing the pain, such as rheumatoid arthritis, a different kind of arthritis that can happen due to a disorder in the immune system.
What Treatments Are There For Osteoarthritis Of The Knee?
Let us now understand how is osteoarthritis of the knee treated? The foremost goal of treating osteoarthritis of the knee are to relieve the pain and recover mobility. The treatment plan will typically include a combination of the following:
1.Weight Loss: For every extra pound on the body an extra three pounds of pressure is exerted on the weight-bearing knee joint. Gaining 10 pounds can mean 30 pounds more pressure on the knee with each step, as well as a significantly greater chance of developing osteoarthritis. So, for people who are overweight or obese, losing weight will significantly reduce pressure and strain on the knee joint. This will alleviate symptoms and perhaps slow down progression of the knee osteoarthritis.
2. Exercise: A variety of exercises, such as strength training, aerobics, range of motion and tai chi, can help with both pain and physical function in knee OA. Strengthening the muscles around the knee makes the joint more stable and decreases pain. Stretching exercises help keep the knee joint mobile and flexible. Water-based exercises may improve function in both knee and hip joints, but offer only minor benefits for pain.
Useful Related Post: Does Exercise Help Treat Arthritis?
3. Physical And Occupational Therapy: If you are having trouble with daily activities, physical or occupational therapy can help. Physical therapists teach you ways to strengthen muscles and increase flexibility in your joint. Occupational therapists teach you ways to perform regular, daily activities, such as housework, with less pain.
4. Pain Relievers And Anti-Inflammatory Drugs. This includes over-the-counter choices. However, don’t take over-the-counter medicines for more than 10 days without checking with your doctor. Taking them for longer increases the chances of side effects. If over-the-counter medications don’t provide relief, your doctor may give you a prescription anti-inflammatory drug or other medication to help ease the pain.
Useful Related Post:What Treatments Are There For Osteoarthritis Of The Knee?
5. Injections are sometimes given directly into a particularly painful knee joint. Two types of injections are commonly used for treatment of severe pain from knee osteoarthritis. Steroid injections and hyaluronic acid injections. Steroids are powerful anti-inflammatory drugs. Hyaluronic acid is normally present in joints as a type of lubricating fluid.
(i) The aim of steroid injections is to reduce swelling and thereby alleviate knee stiffness and pain. Read more about Steroid Injections for Knee Osteoarthritis here.
(ii) The aim of hyaluronic acid injections, known as viscosupplementation, is to provide lubrication for the knee joint. The hyaluronic acid mimics the viscous synovial fluid that naturally lubricates the knee joint.
Read more about Viscosupplementation for Knee Osteoarthritis here.
The degree of pain relief from injections is variable. If effective, the results from the injections are temporary, sometimes lasting up to 6 to12 months.
6. Alternative Therapies: Some alternative therapies that may be effective include topical creams with capsaicin, acupuncture, or supplements, including glucosamine and chondroitin or SAMe.
7. Using Devices Such As Braces: Knee braces are becoming more popular and more evidence to support their use for osteoarthritis is emerging. There are broadly two types of braces that can help to stabilize the kneecap and make it move correctly. “Unloader” type braces can take the weight away from the side of the knee affected by arthritis. And “Support” type braces can provide support for the entire knee. You can buy knee braces from sports shops and chemists. But you should speak to your doctor or physiotherapist first. They may also be able to provide braces or recommend the best ones for you.
8. Knee Surgery: if osteoarthritis symptoms are severe and other treatments don’t succeed, knee replacement surgery may be a treatment option. However, in majority of the cases knee osteoarthritis may never need surgery. Learn here about which surgical options are optimal for treating osteoarthritis in your knee.
(i) Knee Arthroscopy to remove loose pieces of cartilage. Arthroscopy uses a small telescope (arthroscope) and other small instruments. The surgery is done through small incisions. The surgeon uses the arthroscope to look into the joint space. Once there, the surgeon can remove damaged cartilage or loose particles, clean the bone surface, and repair other types of tissue if those damages are discovered. The procedure is often used on younger patients (ages 55 and younger) in order to delay more serious surgery.
Note: In the arthritic knee, there is a very limited role for an arthroscopy. Results of a “clean out” or a “wash out” are unpredictable at best and should be avoided.
(ii) Knee Osteotomy: This procedure involves cutting the bone and reorienting the alignment of the knee. It has traditionally been reserved for younger patients with maligned knees who participate in high-demand activities such as sports. Osteotomy has fallen out of favor due to inferior results compared to knee replacements. There are some newer technologies that may improve outcomes, but currently osteotomy has a limited role in the treatment of osteoarthritis of the knee.
(iii) Knee Arthroplasty: It’s a joint replacement surgery. It’s a surgical procedure in which joints are replaced with artificial parts made from metals or plastic. The replacement could involve one side of the knee or the entire knee. Joint replacement surgery is usually reserved for people over age 50 with severe osteoarthritis. The surgery may need to be repeated later if the joint wears out again after several years, but with today’s modern advancements most new joints will last over 20 years. The surgery has risks, but the results are generally very good.
Learn here all about the surgery options to treat knee osteoarthritis in your knee.
As everyone knows any surgery is a relatively involved procedure and may require a long recovery and rehabilitation period. For most patients, commitment to an extensive and rigorous non-surgical treatment program, which typically includes rehabilitative physical therapy and exercise, may help them avoid the need for knee surgery.

As a former dancer and figure skater, I worry that I may one day develop this… The creaky knees have already started!
I was diagnosed in June, 2013 with OSTEOARTHRITIS of the spine and both knees, symptoms started with severe back pain, joint swelling and stiffness in my knees and eventually the feeling spread to my shoulders and neck, i couldn’t lift my arm without pain medications. I was prescribed tramacet and arcoxia for 8 months but had to stop them due to bad effects. In 2017, I started on OSTEOARTHRITIS HERBAL FORMULA from RICH HERBS FOUNDATION, this natural herbal treatment reversed my osteoarthritis.